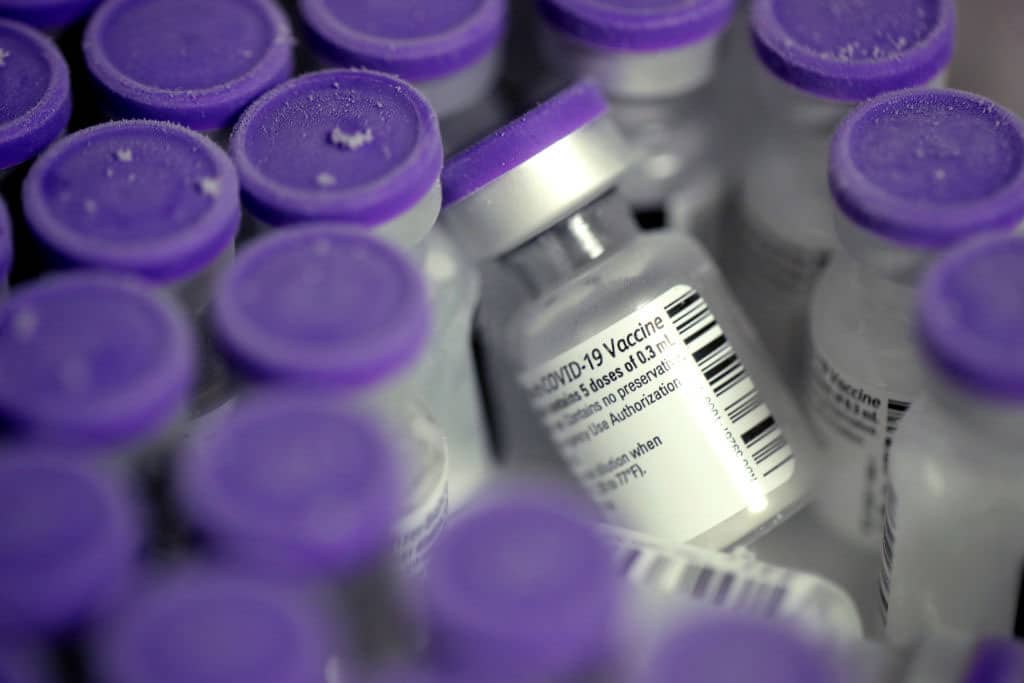
 (Photo by Scott Olson/Getty Images)
(Photo by Scott Olson/Getty Images) The COVID-19 pandemic poses an epic battle between two of nature’s powerful forces: inconceivable numbers of replicating viruses versus a species whose tool-making ingenuity has controlled its destiny and altered the planet.
Until the last few weeks, our strategy against the coronavirus hinged on avoidance: masking and distancing. Now we, the tool makers, are playing “the ace in our deck”: a series of vaccines heralded by two remarkable examples — Pfizer and Moderna — that allow us to immunize ourselves. But the emergence of more contagious strains means that the goal of “herd immunity” — the percentage of immune individuals in the population needed to halt viral spread — has become higher and more difficult to achieve. Will the vaccines now allow us to prevail?
Unfortunately, the virus will continue to circulate and create harm if enough susceptible individuals remain unvaccinated to allow the virus to continue to spread. Here are a few challenges and misinformed arguments we must dispel to successfully reach herd immunity.
The “I Was Already Infected and now Am Immune” Argument
Natural infection does appear to provide protection for at least 90 days. But individuals with mild infections may not develop sufficient antibodies for longer term protection. And the potential for reinfection still looms, potentially allowing the virus to continually re-circulate. Given the possibility of reinfection, we cannot depend on catching COVID-19 and getting sufficient immune protection to reach herd immunity.
As the vaccine is new, we’re also uncertain of the duration of the immunity it confers. However, the high levels of antibodies against COVID-19 produced by the vaccine suggest that the immunity it provides may prove more durable than immunity from natural infection. Vaccination also allows us to systematically track the duration of the response and schedule re-vaccinations as needed. Vaccines can also be adapted to new strains based on the evolution of the virus and monitoring vaccine responses. Natural immunity cannot.
The “Vaccine Isn’t Safe” Argument
The safety issue is not controversial in scientific circles. The technology was jumpstarted by vaccine development for the SARS-1 epidemic of 2002 and the MERS outbreak of 2012. Although SARS-1 proved to be short-lived, the biologic processes underlying the SARS-1 and COVID-19 vaccines are well understood. M-RNA, the active component of the vaccine, is part of the body’s normal cellular system and produces the body’s own proteins. The m-RNA provided by the vaccine, like the body’s own, lasts for only a few days prior to degradation. During that period, it generates the proteins that serve as the stimulus to antibody production, leaving behind antibodies just like those produced by conventional vaccines. These antibodies attack the “spike protein” of the virus, which is the component that attaches to human cells. Without an effective spike protein, the virus becomes neutralized, aborting infection.
The safety profile of the COVID-19 vaccination was established by clinical trials involving tens of thousands of subjects. Reactions to the virus during these trials proved no more problematic than the side effects of common vaccines in everyday use. My own institution, Cedars Sinai, has vaccinated over twelve thousand healthcare providers, myself included, with side effects noted only in very rare cases.
My own institution has vaccinated over twelve thousand healthcare providers with side effects noted only in very rare cases.
Could the vaccine produce unexpected long-term side effects that might not yet be apparent? It simply hasn’t been around long enough to be certain. However, based on the current knowledge of this vaccine and our many decades of medical experience with other vaccines, there would be no reason to expect such untoward effects. The alternative to taking the vaccine — subjecting oneself to the ongoing risk of a potentially deadly infection — poses substantially higher risks.
The Long-Term Challenge
The pervasive fears about the COVID-19 vaccine suggest that the long-term challenge will be convincing skeptical Americans that vaccination protects themselves and others and will move us toward “herd immunity” and a re-opening of society.
Why should the appeal to help end this scourge, based on solid evidence, prove so difficult? In the 1950s, annual polio deaths averaged less than 1% of the COVID 19 toll, and yet, the public’s rapid acceptance of the vaccine drove polio to near extinction. Unfortunately, since that time, social and conventional media re-fashioned a society in which scientific truth, whether in climate change, politics or public health matters, often proves no more influential than unsupported opinions.
Now is the time to heed the call of our legacy of ingenuity, embrace this innovative vaccine and end the suffering. We all need to answer this “call to arms” and vaccinate ourselves while encouraging our friends and neighbors to do so as well. The closer we get to universal vaccination, the better our future will be.
Daniel Stone is Regional Medical Director of Cedars-Sinai Valley Network and a practicing internist and geriatrician with Cedars Sinai Medical Group. The views expressed in this column do not necessarily reflect those of Cedars-Sinai.























 More news and opinions than at a Shabbat dinner, right in your inbox.
More news and opinions than at a Shabbat dinner, right in your inbox.