
Category
icu

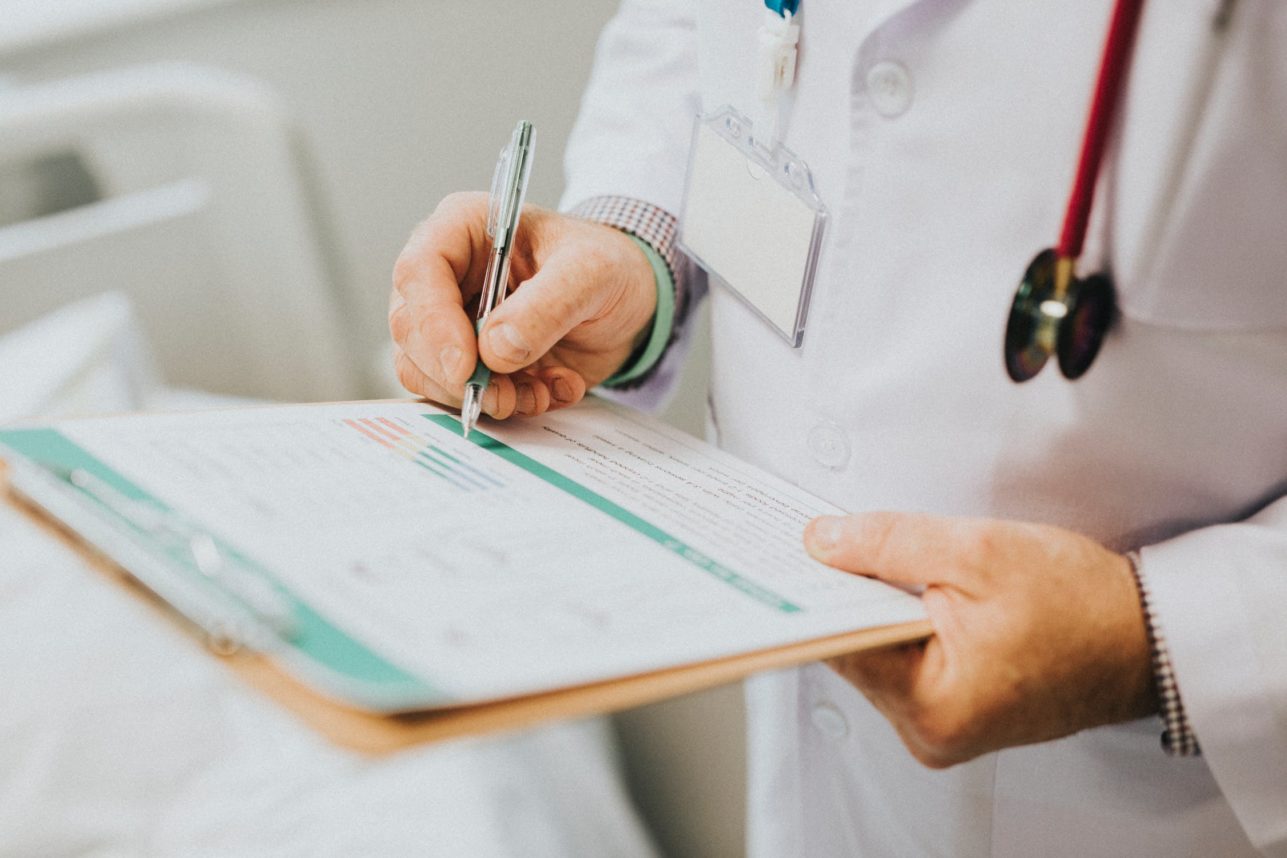
NYC Health Department: Yeshivas Must Exclude Unvaccinated Students or Risk Being Shut Down
Erin Ben-Moche
April 8, 2019
When it’s time to die
Jewish Journal
October 7, 2015
A recent study of critical-care physicians at one Southern California hospital system found that more than 1 in 10 patients receiving treatment in their hospitals’ intensive care units were receiving treatments that would not benefit the patient in a meaningful way.
Religion rarely part of ICU conversation
Jewish Journal
August 31, 2015
In less than 20 percent of family meetings in the intensive care unit do doctors and other health care providers discuss religion or spirituality a new study finds.
My Mother’s Mostly Beautiful Heart
Reeva Hunter Mandelbaum
May 11, 2006
\”Overall, she has a mostly beautiful heart\” is what the cardiologist, my brother\’s friend, says
New Articles

Nova Festival Exhibit in Manhattan Harrowing and Inspiring
Alan Zeitlin
April 26, 2024

Steve Garvey Holds Press Conference Calling for Action Against Pro-Palestinian Campus Protests
Aaron Bandler
April 25, 2024

West Hollywood’s MASH Gallery Exhibition to Feature Female Jewish Art
Brian Fishbach
April 25, 2024

Echad Mi Yodea? Who Knows One?
Rick Lupert
April 25, 2024

The First Alphabet and the Third Plague
Gershon Hepner
April 25, 2024
 More news and opinions than at a Shabbat dinner, right in your inbox.
More news and opinions than at a Shabbat dinner, right in your inbox.